Intradiscal RFA-Biacuplasty
When back pain originates inside the disc itself (not from a pinched nerve) most standard treatments miss the target. Intradiscal RFA-Biacuplasty heats the disc from within to destroy the pain receptors at the source.
Your journey
Your Road to a Pain-Free Life
Test your knowledge
How Well Do You Know This Procedure?
Frequently asked questions
What is Intradiscal RFA-Biacuplasty?
Intradiscal RFA-Biacuplasty is a minimally invasive procedure designed to treat pain that originates from inside an intervertebral disc. Two radiofrequency electrodes are placed into the painful disc (one on each side) through small needle punctures. Bipolar radiofrequency energy is then applied between the two probes. The controlled heat destroys the nociceptors (pain receptors) in the disc's outer wall (the annulus fibrosus) and causes gentle thermal remodelling of the disc tissue.
What is discogenic pain?
Discogenic pain means the disc itself is the source of pain (not a pinched nerve. Over time, discs can develop small tears in their outer wall (the annulus fibrosus). Pain-sensitive nerve fibres grow into these tears and become chronically inflamed. The result is a deep, aching back pain that is worse with prolonged sitting, bending forward, or lifting. MRI often shows characteristic changes) such as Modic endplate changes, a high-intensity zone (HIZ), or annular fissures.
Who is a candidate for Intradiscal RFA-Biacuplasty?
Ideal candidates have chronic axial (central) low back pain predominantly from one or two disc levels, confirmed by MRI (Modic changes, annular tear, or HIZ). They have not had adequate relief from conservative treatments, physiotherapy, medications, and epidural steroid injections. Discography may be performed to confirm the exact pain-generating disc before proceeding. Biacuplasty is not suitable for patients with large disc herniations pressing on nerve roots.
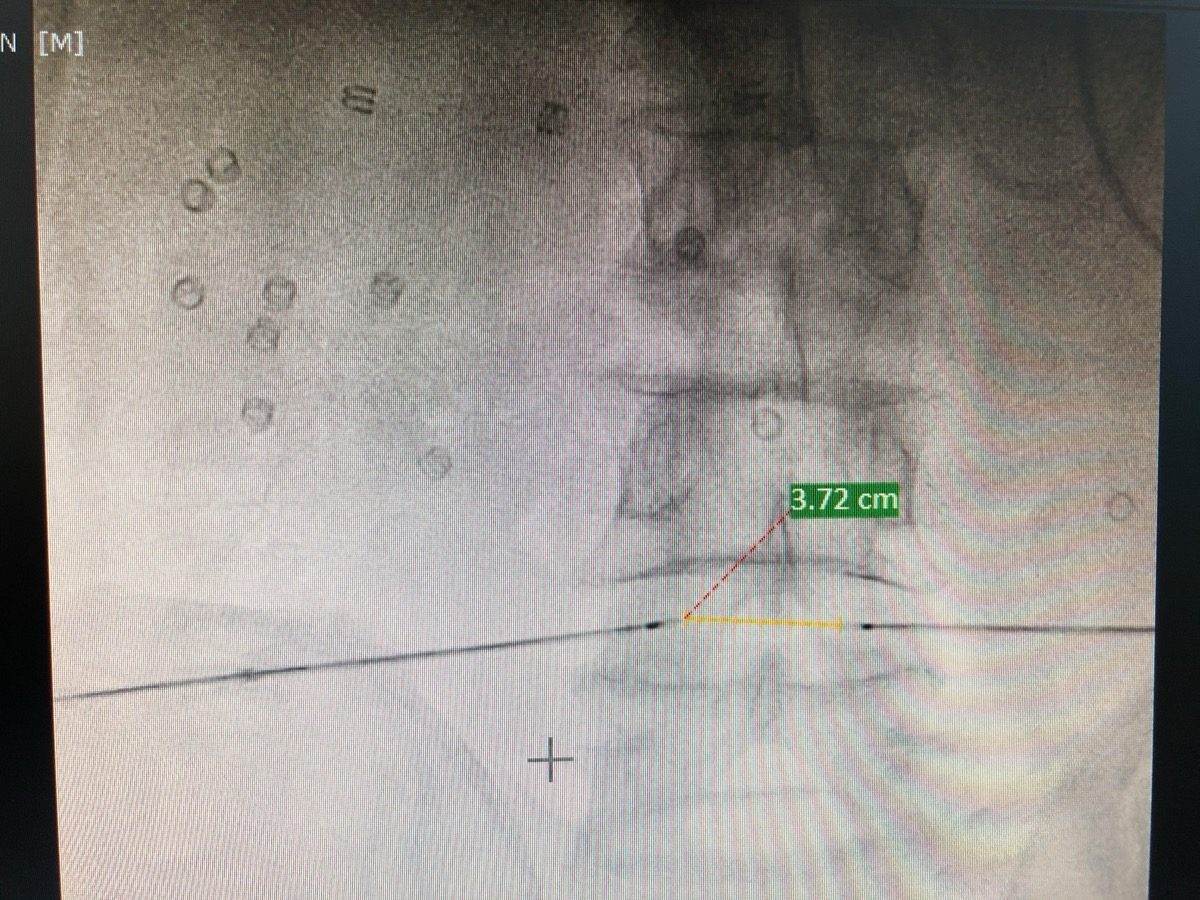
How is Intradiscal RFA-Biacuplasty performed?
You lie face-down. Under fluoroscopy guidance, two RF probe needles are introduced into the affected disc through a posterolateral (oblique) approach, one from the left side, one from the right. Contrast dye confirms correct intradiscal placement. The two probes create a bipolar RF circuit. Controlled heat is applied across both electrodes for approximately 15 minutes. The heat ablates the pain fibres in the annulus without damaging the nucleus or the nerve roots. The procedure takes 35–50 minutes in total.
Is this the same as an epidural steroid injection?
No. They are fundamentally different. An epidural steroid injection targets nerve root inflammation outside the disc, in the epidural space. It is most effective for radiculopathy (pain radiating down the leg due to a compressed nerve). Biacuplasty works inside the disc to destroy the nociceptors in the disc wall. It addresses disc-sourced axial back pain, not nerve root compression.
When will I feel better after Intradiscal RFA-Biacuplasty?
Relief is gradual. Expect mild disc soreness for 1–2 weeks post-procedure. Pain reduction typically begins around 4–6 weeks as the treated disc settles. Full benefit is usually felt at 8–12 weeks. Patients are encouraged to start core strengthening exercises as soon as the initial soreness resolves.
Are there any risks of Intradiscal RFA-Biacuplasty?
As with any intradiscal procedure, the main risks are discitis (disc infection) and temporary worsening of back pain during the immediate post-procedure period. Prophylactic antibiotics are given to minimise infection risk. The procedure is performed under strict sterile conditions. Serious complications such as nerve injury or disc damage are rare. Dr. Jain will discuss all risks in detail during the consent process.
Any concern?