Sciatica: Causes, Symptoms, and Treatment Options
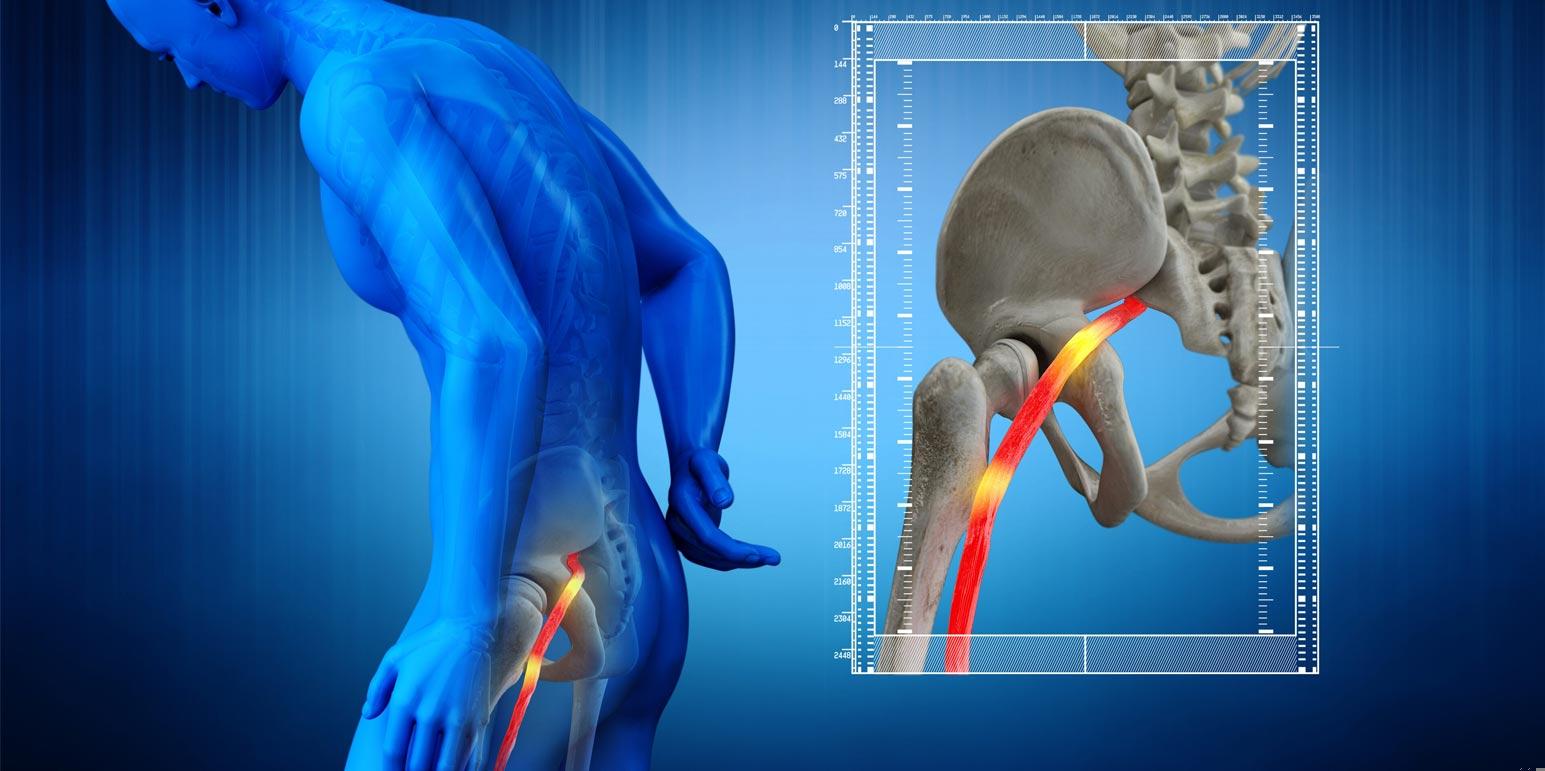
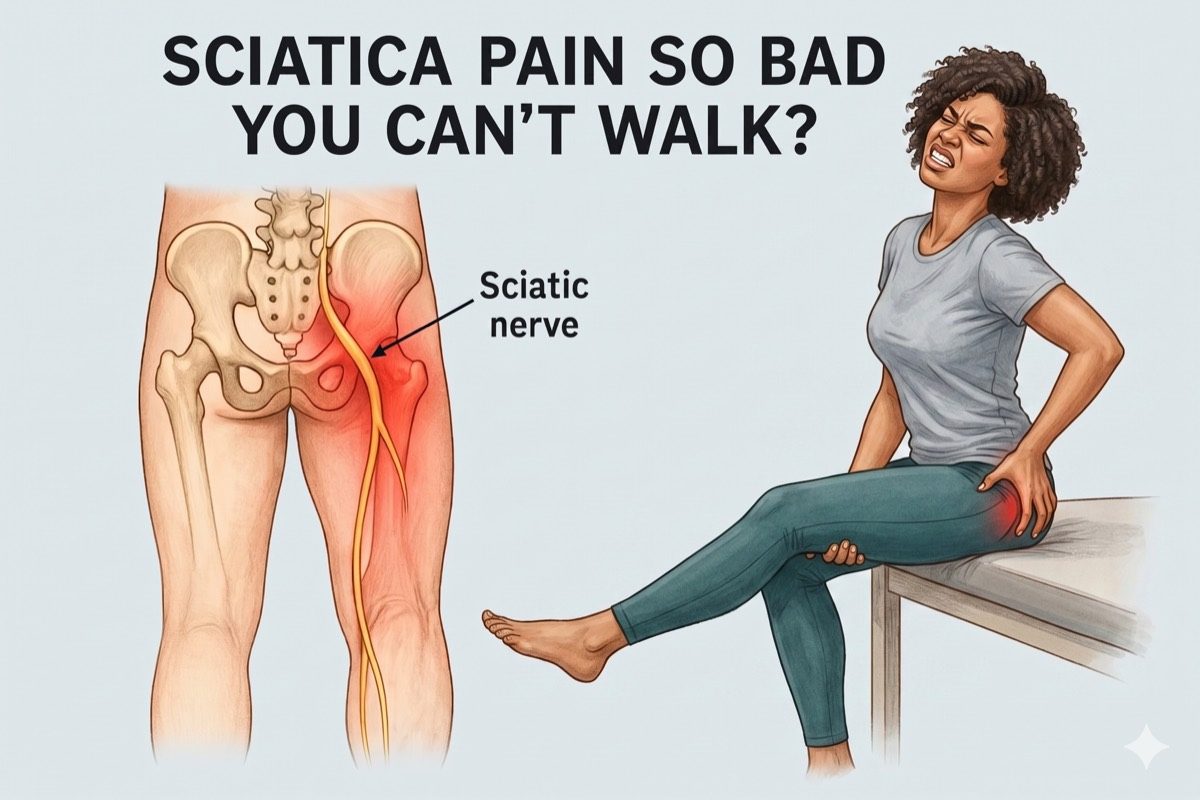
Sciatica causes sharp, shooting pain that travels from the lower back down one leg. It can make sitting, walking, and sleeping very difficult. The good news is that most cases respond well to the right treatment.
The sciatic nerve is the longest nerve in the body. It starts in the lower back, runs through the buttock, and goes all the way down the leg. When this nerve gets compressed or irritated, it causes sciatica.
What is Sciatica?
Sciatica is not a condition on its own. It is a symptom of an underlying problem in the spine or pelvis that is pressing on the sciatic nerve or its roots.
It usually affects one leg at a time. The pain can be mild or severe, and it often gets worse after sitting for a long time or making certain movements.
Most people with sciatica get better with the right treatment. Surgery is rarely needed.

Symptoms of Sciatica
The most common symptom is pain that starts in the lower back and travels down one leg. You may also feel:
- A burning or electric shock sensation down the leg
- Numbness or tingling in the leg or foot
- Weakness in the leg or difficulty moving it
- Pain that gets worse when sitting, coughing, or sneezing
In rare cases, sciatica can cause loss of bladder or bowel control. This needs immediate medical attention.
What Causes Sciatica?
Sciatica happens when something presses on the sciatic nerve. The most common causes are:
- Herniated disc: A disc in the spine bulges out and presses on the nerve root
- Spinal stenosis: Narrowing of the spinal canal that squeezes the nerves
- Piriformis syndrome: A deep buttock muscle that tightens and irritates the sciatic nerve
- Spondylolisthesis: A vertebra slips forward and pinches the nerve
- Degenerative disc disease: Worn discs that put pressure on nearby nerves
Risk factors include prolonged sitting, heavy lifting with poor posture, excess body weight, and age-related changes in the spine.
Piriformis Syndrome
The piriformis is a small muscle deep in the buttock. When it becomes tight or inflamed, it can press directly on the sciatic nerve.
This condition is often missed because the symptoms look exactly like disc-related sciatica. A careful physical examination and targeted nerve block can help confirm the diagnosis.
Treatment for piriformis syndrome differs from spinal sciatica, so getting the right diagnosis matters.
How is Sciatica Diagnosed?
A thorough diagnosis includes a physical examination, medical history, and imaging. Your doctor will look for the source of nerve compression.
Common diagnostic steps include:
- Straight leg raise test to identify nerve tension
- MRI scan to visualise disc herniations and nerve compression
- X-rays to rule out bone spurs or alignment issues
- Nerve conduction studies in complex cases
- Diagnostic nerve blocks to confirm the pain source
Check If You Need This Treatment
What we offer?
Our approach to treating sciatica
We use targeted, minimally invasive procedures that go directly to the source of the pain.
-
Transforaminal Epidural Steroid Injection (TFESI) to reduce nerve root inflammation
-
Caudal Epidural Injection for widespread lumbar nerve involvement
-
Dorsal Root Ganglion (DRG) Pulsed Radiofrequency Ablation (RFA) for long-term pain relief
-
Piriformis Muscle Injection for piriformis syndrome
-
In-house MRI, X-ray, and nerve conduction studies for accurate diagnosis
Frequently asked questions
What are the main causes of sciatica?
The most common cause is a herniated disc pressing on a nerve root. Other causes include spinal stenosis, piriformis syndrome, and spondylolisthesis. A proper MRI and physical examination will confirm the exact cause.
How is sciatica diagnosed?
Diagnosis involves a physical examination, straight leg raise test, and imaging. An MRI is the most useful scan to identify disc herniations and nerve compression. In some cases, nerve conduction studies or diagnostic nerve blocks are used.
What interventional treatments are available for sciatica?
We offer Transforaminal Epidural Steroid Injections (TFESI), Caudal Epidural Injections, Dorsal Root Ganglion (DRG) Pulsed RFA, and Piriformis Muscle Injections. The right procedure depends on the cause and severity of your sciatica.
How long does it take to recover from sciatica?
Most patients with mild to moderate sciatica improve within 4 to 6 weeks. With interventional procedures, many patients experience significant relief within days to weeks. Severe cases may need a longer tailored treatment plan.
Can sciatica come back after treatment?
Yes, sciatica can return if the underlying cause is not addressed. Maintaining a healthy weight, doing targeted exercises, and avoiding prolonged sitting helps reduce the risk of recurrence. Regular follow-up with your pain specialist is important.
When should I see a specialist for sciatica?
See a pain specialist if your pain has lasted more than 4 weeks, if it is severe or worsening, or if you have numbness or weakness in the leg. Immediate care is needed if you lose bladder or bowel control.
Is surgery always needed for sciatica?
Surgery is rarely needed. Most patients get good relief from interventional procedures such as epidural steroid injections or RFA. Surgery is only considered when there is significant nerve compression causing progressive weakness, or when all other treatments have failed.
Any concern?