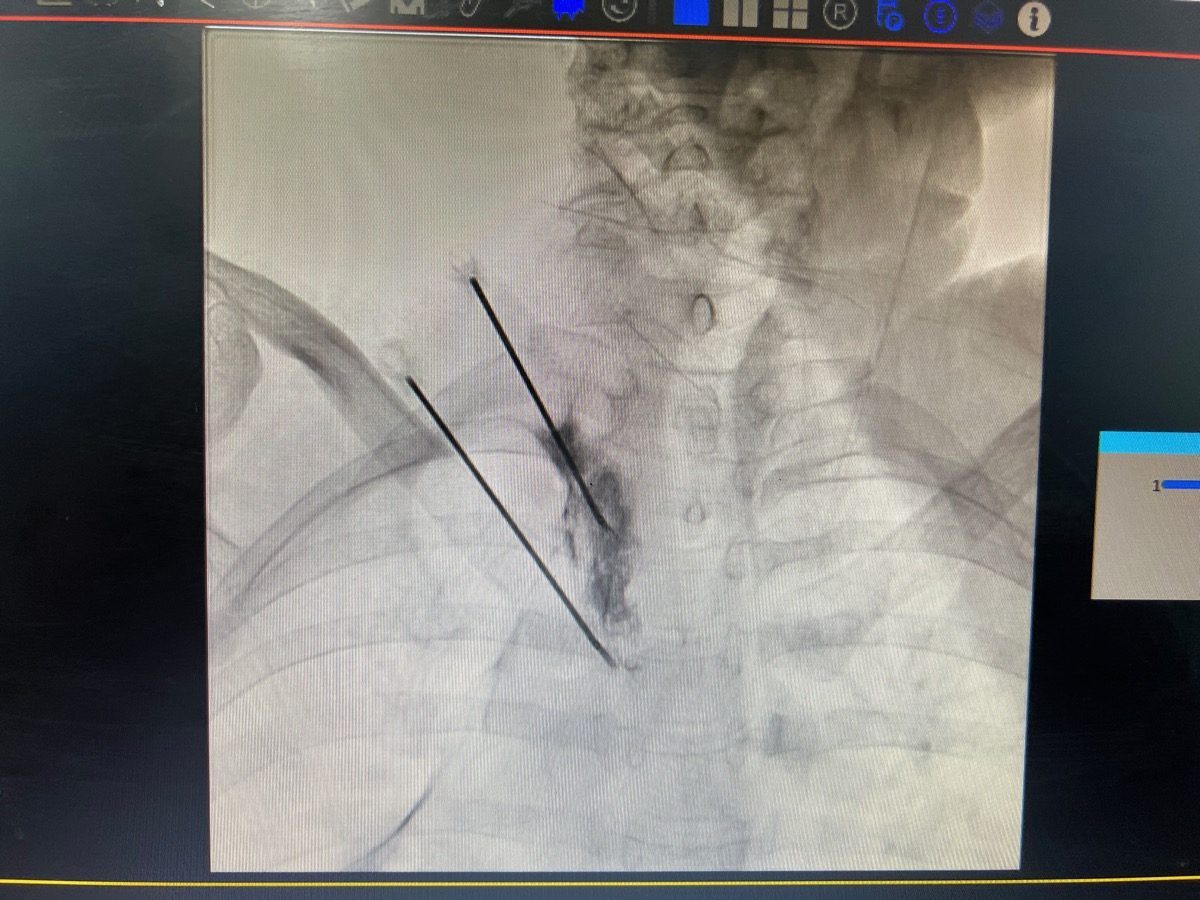
Sympathectomy & Sympathetic Nerve Blocks
Some pain conditions are driven by the sympathetic nervous system, the involuntary nerve network that controls blood flow, sweating, and organ function. A targeted sympathetic nerve block or sympathectomy interrupts these abnormal pain signals at their source.
Your journey
Your Road to a Pain-Free Life
Test your knowledge
How Well Do You Know This Procedure?
Frequently asked questions
What is the sympathetic nervous system, and what is a sympathectomy?
The sympathetic nervous system is the involuntary ("fight or flight") part of the nervous system. It regulates blood vessel tone, sweating, and organ function. In certain pain conditions (particularly CRPS (complex regional pain syndrome), peripheral vascular disease, and hyperhidrosis) the sympathetic nerves become abnormally overactive. A sympathectomy interrupts or destroys a portion of the sympathetic chain, breaking this abnormal cycle. A sympathetic nerve block uses local anaesthetic to temporarily interrupt the same pathways, useful diagnostically and therapeutically.
What conditions can be treated with sympathetic blocks or sympathectomy?
Several conditions respond to sympathetic intervention:
Stellate Ganglion Block (cervical): CRPS of the arm or hand, post-mastectomy hot flushes, some cardiac arrhythmias, facial sympathetically-mediated pain.
Lumbar Sympathetic Block: CRPS of the leg or foot, peripheral arterial disease with ischaemic pain, hyperhidrosis of the lower limbs.
Coeliac Plexus Block: Upper abdominal cancer pain (pancreatic, gastric, hepatic), chronic pancreatitis pain.
Thoracic Sympathectomy: Palmar hyperhidrosis (excessive sweating of the palms), facial blushing, CRPS of the upper extremity.
How is a sympathetic block or sympathectomy performed?
All procedures are done under fluoroscopic or ultrasound guidance with the patient on an imaging table. The specific approach depends on the target:
Stellate ganglion: Ultrasound-guided needle to the anterolateral neck at C6, anterior to the longus colli muscle. Local anaesthetic injected.
Lumbar sympathetic: Fluoroscopy-guided needle to the anterolateral surface of the L2–L4 vertebral bodies. LA or a neurolytic agent (phenol or alcohol) is used.
Coeliac plexus: Fluoroscopy or CT-guided bilateral needles to the coeliac axis at T12–L1. Neurolysis with absolute alcohol for cancer pain gives prolonged relief.
For longer-lasting effect without neurolytic agents, RF sympathectomy ablates the sympathetic ganglia using radiofrequency energy.
What does a diagnostic sympathetic block tell us about your pain?
A diagnostic sympathetic block uses only local anaesthetic. Its purpose is to determine whether your pain has a sympathetically-maintained component. If you achieve ≥50% relief after a successful block (confirmed by objective signs such as a temperature rise in the limb after lumbar sympathetic block, or a Horner's syndrome after stellate block), then a longer-lasting sympathectomy is likely to benefit you. Patients who do not respond to a diagnostic block are unlikely to respond to sympathectomy.
What should I expect after a lumbar sympathetic block?
After a successful lumbar sympathetic block, the treated leg will feel warm, and the skin colour may improve (more pink/flushed). This warmth is a sign that the blood vessels in the limb have dilated, confirming the sympathetic nerves have been blocked. Pain relief may be noticed over minutes to hours. Some mild back discomfort at the injection site resolves in 24–48 hours. You will need a driver home, as the leg may feel heavy for a few hours.
How long does pain relief last after a sympathetic block or sympathectomy?
A diagnostic block with local anaesthetic lasts hours to days. A neurolytic sympathectomy (using phenol or alcohol) typically lasts 3–6 months. RF sympathectomy lasts 6–18 months. For coeliac plexus neurolysis with absolute alcohol in cancer pain, relief can persist for months and often matches the disease trajectory. Procedures can be repeated if pain returns.
Are there any side effects unique to sympathetic procedures?
Each procedure has specific considerations:
Stellate ganglion block: Horner's syndrome (drooping eyelid, small pupil, reduced sweating on one side of face), temporary and expected, confirms correct block. Hoarseness, temporary arm heaviness.
Lumbar sympathetic: Compensatory sweating (increased sweating in untreated areas), temporary leg heaviness or warmth.
Thoracic sympathectomy: Compensatory hyperhidrosis (sweating shifts to the trunk or groin) is the most commonly noted side effect; severity varies.
Coeliac plexus block: Temporary diarrhoea and orthostatic hypotension (dizziness on standing) in the first 24–48 hours. Serious complications are rare.
Any concern?